Placenta Previa: Pathogenesis and Clinical Findings
Authors: Wendy Yao, Yan Yu* Reviewers: Danielle Chang, Crystal Liu, Aysah Amath* * MD at time of publication
Note on Physical Exam:
• Do not perform bimanual exam during vaginal bleed until placenta previa is ruled out (2nd trimester onwards)
• If patient presents with bleeding, a pelvic exam = risk of damaging placentaàmore bleeding
• Use transvaginal ultrasound to confirm location of placenta
Previous C/S Multiple gestation Maternal smoking
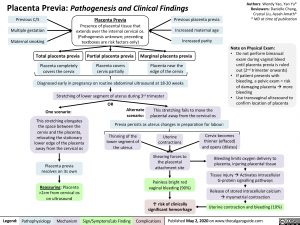
Placenta Previa
Presence of placental tissue that extends over the internal cervical os. (Pathogenesis unknown; preceding textboxes are risk factors only)
Previous placenta previa Increased maternal age Increased parity
Total placenta previa
Placenta completely covers the cervix
Partial placenta previa
Placenta covers cervix partially
Marginal placenta previa
Placenta near the edge of the cervix
Diagnosed early in pregnancy on routine abdominal ultrasound at 18-20 weeks Stretching of lower segment of uterus during 3rd trimester
OR
Alternate scenario:
One scenario:
This stretching elongates the space between the cervix and the placenta, relocating the stationary lower edge of the placenta away from the cervical os
Placenta previa resolves on its own
Reassuring: Placenta >2cm from cervical os on ultrasound
This stretching fails to move the placental away from the cervical os
Previa persists as uterus changes in preparation for labour:
Thinning of the lower segment of the uterus
Uterine contractions
Shearing forces to the placental attachment site
Painless bright red vaginal bleeding (90%)
↑ risk of clinically significant hemorrhage
Cervix becomes thinner (effaced) and opens (dilates)
Bleeding limits oxygen delivery to placenta, injuring placental tissue
Tissue injuryàActivates intracellular G-protein signalling pathways
Release of stored intracellular calcium àmyometrial contraction
Uterine contraction and bleeding (10%)
Legend:
Pathophysiology
Mechanism
Sign/Symptom/Lab Finding
Complications
Published May 2, 2020 on www.thecalgaryguide.com
Foundations
Systems
Other Languages
Obstetrics 3rd Trimester Bleeding Placenta Previa: Pathogenesis and Clinical Findings Placenta-Previa