Diverticulosis and Angiodysplasia:
Pathogenesis and Clinical Features
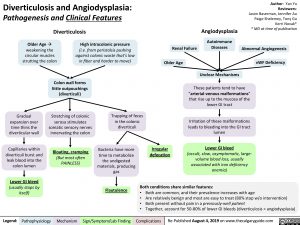
Diverticulosis
Author: Yan Yu Reviewers: Jason Baserman, Jennifer Au Paige Shelemey, Tony Gu Kerri Novak* * MD at time of publication
Abnormal Angiogenesis
vWF Deficiency
Older Ageà weakening the circular muscles strutting the colon
High intracolonic pressure
(i.e. from peristalsis pushing against colonic waste that’s low in fiber and harder to move)
Angiodysplasia
Autoimmune Diseases
Unclear Mechanisms
These patients tend to have “arterial-venous malformations” that rise up to the mucosa of the lower GI tract
Irritation of these malformations leads to bleeding into the GI tract lumen
Lower GI bleed
(occult, slow, asymptomatic, large- volume blood loss, usually associated with iron deficiency anemia)
Renal Failure
Older Age
Gradual expansion over
time thins the diverticular wall
Capillaries within diverticuli burst and leak blood into the colon lumen
Lower GI bleed
(usually stops by itself)
Colon wall forms little outpouchings (diverticuli)
Stretching of colonic serosa stimulates
somatic sensory nerves innervating the colon
Bloating, cramping
(But most often PAINLESS)
Trapping of feces in the colonic diverticuli
Bacteria have more time to metabolize the undigested materials, producing gas
Flautulence
Irregular defecation
Both conditions share similar features:
• Both are common, and their prevalence increases with age
• Are relatively benign and most are easy to treat (80% stop w/o intervention)
• Both present without pain in a previously-well patient
• Together, account for 50-80% of lower GI bleeds (diverticulosis > angiodysplasia)
Legend:
Pathophysiology
Mechanism
Sign/Symptom/Lab Finding
Complications
Re-Published August 4, 2019 on www.thecalgaryguide.com