SEARCH RESULTS FOR: Inflammatory-Versus-Degenerative-Joint-Disease
Inflammatory Versus Degenerative Joint Disease
 1hr
after waking
Legend: Mechanism
Sign/Symptom/Lab Finding Systemic
immune
activation occurs
↑
Inflammatory
mediators
circulate
throughout the
body
Extra-
articular
involvement
(e.g., skin,
eyes, lung,
heart,
kidneys) ±
abnormal
inflammatory
markers (CRP,
ESR) &
autoantibodi
es (RF, ANA)
Pathophysiology Complications
Degenerative Joint Disease
Abnormal mechanics or repetitive/excessive
loading stresses the joints
Joint structures degrade over time
Movement
(using the
joint)
exacerbates
the
mechanical
forces that are
wearing down
the joint
Pain with
movement
Pain relieved
with rest
Fragments of broken
articular cartilage
triggers a mild
synovial (thin lining
inside of the joint)
inflammation that
seeps fluid into the
synovial membrane
during inactivity
Joints stiffen with rest
Moving the joint
physically pushes
inflammatory fluid
back into lymphatic
vessels (body's clean-
up system) within
minutes
Joint stiffness resolves
within minutes of
movement
Published on www.thecalgaryguide.com
Authors:
Yan Yu
Mackenzie Trpcic
Reviewers:
Jennifer Au
Sean Spence
Martin Atkinson*
Catherine R Jarvis
* MD at time of
publication
The weight-
bearing joints
(i.e., knee, hip, &
lumbar/cervical
facet joints)
sustain the
highest
mechanical load
& degeneration
Distinguishing between Inflammatory and Degenerative joint disease
Inflammatory Joint
Disease
Auto-immune attack of body tissues, due to
failure of the body’s immune system to
discriminate between self and non-self.
Degenerative Joint
Disease
Repetitive, excess, or abnormal mechanical
forces on joints over time, leading to physical
breakdown of the joint.
Authors:
Yan Yu
Reviewers:
Jennifer Au
Sean Spence
Martin Atkinson*
* MD at time of
publication
Within joints, severe synovial inflammation
dilates local blood vessels, and causes the
vessel endothelium to be more leaky.
Accumulation of abundant
inflammatory synovial fluid
at rest or overnight
Swelling stimulates
joint nociceptors
Pain with rest
Moving the joint
physically pushes fluid
back into lymphatics,
relieving the painful
swelling.
Pain relieved with
motion
Legend: Overnight fluid
accumulation in the
synovial membrane
Morning stiffness
Lots of fluid, takes
more time (hours)
to be reabsorbed
by lymphatics
Stiffness resolves
after >1hr
Blood carries
heat and
looks red
Warm, Red,
Swollen
Joints
Pathophysiology Mechanism
Sign/Symptom/Lab Finding Inflammation is
oftentimes
systemic, not
localized
exclusively within
the joint (i.e. in
Rheumatoid
arthritis, Lupus,
etc)
Extra-articular
manifestations;
positive
inflammatory
markers (CRP,
ESR, RF, ANA)
Motion (using
the joint)
exacerbates the
mechanical
forces that are
wearing down
the joint
Fragments of
broken articular
cartilage triggers a
mild synovial
inflammation that
seeps fluid into the
synovial membrane
during inactivity
Pain with motion
(relieved by rest)
Joint stiffness
after inactivity
Moving the joint physically
pushes inflammatory fluid
back into lymphatics within
minutes.
Note: one big difference btw
the two is the degree of joint
inflammation (synovitis)
present in the joint capsule
Stiffness is short-lived,
quickly relieved by
movement
Published November1,2012 on www.thecalgaryguide.com
Larger, weight-
bearing joints tend to
bear the brunt of the
mechanical forces
Most commonly
affects the knee,
hip, and L/C-spine
facet joints
Complications" title="Legend: Inflammatory vs Degenerative Joint Disease: Pathogenesis & clinical findings
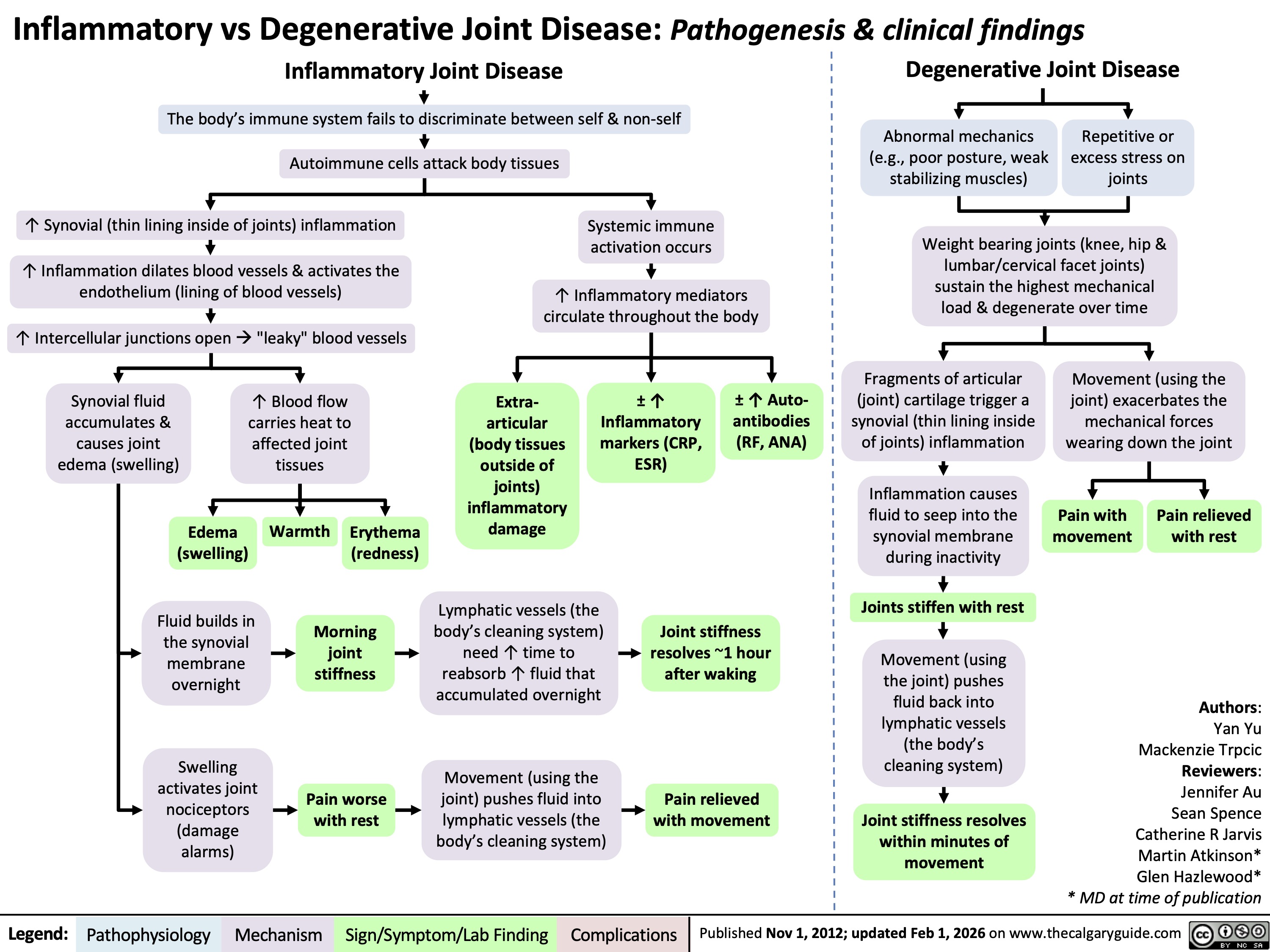
Inflammatory Joint Disease
The body’s immune system fails to discriminate between self & non-self
Autoimmune cells attack body tissues
↑ Synovial (thin lining inside of joints) inflammation
↑ Inflammation dilates blood vessels & activates the
endothelium (lining of blood vessels)
↑ Intercellular junctions open à "leaky" blood vessels
Synovial fluid
accumulates &
causes joint
edema (swelling)
↑ Blood flow
carries heat to
affected joint
tissues
Edema
(swelling)
Warmth
Erythema
(redness)
Fluid builds in
the synovial
membrane
overnight
Morning
joint
stiffness
Swelling
activates joint
nociceptors
(damage
alarms)
Pain worse
with rest
Systemic immune
activation occurs ↑ Inflammatory mediators
circulate throughout the body
Extra-
articular
(body tissues
outside of
joints)
inflammatory
damage
± ↑
Inflammatory
markers (CRP,
ESR)
± ↑ Auto-
antibodies
(RF, ANA)
Lymphatic vessels (the
body’s cleaning system)
need ↑ time to
reabsorb ↑ fluid that
accumulated overnight
Joint stiffness
resolves ~1 hour
after waking
Movement (using the
joint) pushes fluid into
lymphatic vessels (the
body’s cleaning system)
Pain relieved
with movement
Degenerative Joint Disease
Abnormal mechanics
(e.g., poor posture, weak
stabilizing muscles)
Repetitive or
excess stress on
joints
Weight bearing joints (knee, hip &
lumbar/cervical facet joints)
sustain the highest mechanical
load & degenerate over time
Fragments of articular
(joint) cartilage trigger a
synovial (thin lining inside
of joints) inflammation
Movement (using the
joint) exacerbates the
mechanical forces
wearing down the joint
Inflammation causes
fluid to seep into the
synovial membrane
during inactivity
Pain with
movement
Pain relieved
with rest
Joints stiffen with rest
Movement (using
the joint) pushes
fluid back into
lymphatic vessels
(the body’s
cleaning system)
Joint stiffness resolves
within minutes of
movement
Authors:
Yan Yu
Mackenzie Trpcic
Reviewers:
Jennifer Au
Sean Spence
Catherine R Jarvis
Martin Atkinson*
Glen Hazlewood*
* MD at time of publication
Published Nov 1, 2012; updated Feb 1, 2026 on www.thecalgaryguide.com
Pathophysiology Mechanism
Sign/Symptom/Lab Finding Complications
Final slide is the 1st slide
Legend: Inflammatory vs Degenerative Joint Disease: Pathogenesis & clinical findings
Inflammatory Joint Disease
Degenerative Joint Disease
The body’s immune system fails to discriminate between self & non-self
Autoimmune cells attack body tissues
Abnormal mechanics
(e.g., poor posture, weak
stabilizing muscles)
Repetitive or
excess stress on
joints
↑ Synovial (thin lining inside of joints)
inflammation dilates blood vessels
Systemic immune
activation occurs ↑ Endothelium (lining of blood vessels) activation
opens intercellular junctions (“leaky” blood vessels”)
↑ Inflammatory mediators
circulate throughout the body
Weight bearing joints (knee, hip &
lumbar/cervical facet joints)
sustain the highest mechanical
load & degenerate over time
Synovial fluid
accumulates &
causes joint
edema (swelling)
Edema
(swelling)
↑ Blood flow
carries heat to
affected joint
tissues
Extra-
articular
(body tissues
outside of
± ↑
Inflammatory
markers (CRP,
ESR)
± ↑ Auto-
antibodies
(RF, ANA)
Fragments of articular
(joint) cartilage trigger a
synovial (thin lining inside
of joints) inflammation
Movement (using the
joint) exacerbates the
mechanical forces
wearing down the joint
joints)
inflammatory
Inflammation causes
Warmth Pain relieved
Erythema
damage
fluid to seep into the
Pain with
(redness)
synovial membrane
movement
with rest
during inactivity
Fluid builds in
the synovial
membrane
overnight
Morning
joint
stiffness
Lymphatic
vessels (cleaners)
need ↑ time to
reabsorb ↑ fluid
that accumulated
overnight
Joints stiffen
with rest
Joint stiffness resolves
~1 hour after waking
Movement (using
the joint) pushes
fluid back into
lymphatic vessels
(cleaners)
Swelling
activates joint
nociceptors
(damage
alarms)
Pain worse
with rest
Movement (using
the joint) pushes
fluid into
lymphatic vessels
(cleaners)
Pain relieved with
movement
Joint stiffness
resolves within
minutes of
movement
Authors:
Yan Yu
Mackenzie Trpcic
Reviewers:
Jennifer Au
Sean Spence
Martin Atkinson*
Catherine R Jarvis
* MD at time of
publication
Published on www.thecalgaryguide.com
Pathophysiology Mechanism
Sign/Symptom/Lab Finding Complications
Inflammatory vs Degenerative Joint Disease: Pathogenesis & clinical findings
Inflammatory Joint Disease
Degenerative Joint Disease
The body’s immune system fails to discriminate between self & non-self
Auto-immune cells attack body tissues
Abnormal mechanics
(e.g., poor posture, weak
stabilizing muscles)
Repetitive or
excess stress on
joints
↑ Synovial (thin lining inside of joints)
inflammation dilates blood vessels
Systemic immune
activation occurs ↑ Endothelium (lining of blood vessels) activation
opens intercellular junctions (“leaky” blood vessels”)
↑ Inflammatory mediators
circulate throughout the body
Weight bearing joints (knee, hip &
lumbar/cervical facet joints)
sustain the highest mechanical
load & degenerate over time
Synovial fluid accumulates &
leads to joint edema (swelling)
↑ Blood flow carries heat
to affected joint tissues
Swelling
activates
joint
nociceptors
(damage
alarms)
Fluid
builds in
the
synovial
membrane
overnight
Edema
(swelling)
Warmth
Erythema
(redness)
Extra-articular
(body tissues
outside of
joints)
inflammatory
damage
± ↑
Inflammatory
markers (CRP,
ESR) & auto-
antibodies
(RF, ANA)
Movement (using the
joint) exacerbates the
mechanical forces
wearing down the joint
Pain with
movement
Pain relieved
with rest
Pain worse
with rest
Morning
joint stiffness
Movement
(using the
joint) pushes
fluid into
lymphatic
vessels
(cleaners)
Lymphatic
vessels
(cleaners)
need ↑ time
to reabsorb
↑ fluid
overnight
Pain relieved
with
movement
Joint stiffness
resolves ~1 hour
after waking
Authors:
Yan Yu
Mackenzie Trpcic
Reviewers:
Jennifer Au
Sean Spence
Martin Atkinson*
Catherine R Jarvis
* MD at time of
publication
Legend: Pathophysiology Mechanism
Sign/Symptom/Lab Finding Complications
Fragments of articular
(joint) cartilage trigger a
synovial (thin lining inside
of joints) inflammation
Inflammation causes
fluid to seep into the
synovial membrane
during inactivity
Joints stiffen
with rest
Movement (using
the joint) pushes
inflammatory fluid
back into lymphatic
vessels (cleaners)
Joint stiffness
resolves within
minutes of
movement
Published on www.thecalgaryguide.com
Inflammatory vs Degenerative Joint Disease: Pathogenesis & clinical findings
Inflammatory Joint Disease
The body’s immune system fails to discriminate between self and non-self
Auto-immune cells attack body tissues
↑ Synovial (thin lining inside of joints)
inflammation dilates blood vessels
↑ Endothelium (lining inside of
blood vessels) permeability
Synovial fluid accumulates &
leads to joint edema
(swelling)
Systemic immune
activation occurs
↑ Inflammatory mediators
circulate throughout the
body
Extra-articular
involvement
(body tissues
outside of
joints)
Elevated
inflammatory
markers (CRP,
ESR) & auto-
antibodies
(RF, ANA)
Degenerative Joint Disease
Abnormal
mechanics (e.g.,
poor posture,
weak stabilizing
muscles)
Repetitive/excess
stress on joints
Weight bearing joints (knee, hip &
lumbar/cervical facet joints)
sustain the highest mechanical
load & degenerate over time
Movement (using the joint)
exacerbates the mechanical
forces wearing down the
joint
Pain with
movement
Pain
relieved
with
rest
Authors:
Yan Yu
Mackenzie Trpcic
Reviewers:
Jennifer Au
Sean Spence
Martin Atkinson*
Catherine R Jarvis
* MD at time of
publication
Swelling activates
pain-sensitive joint
nociceptors
(damage alarms)
Pain worse with rest
Joint movement
pushes fluid into
lymphatic vessels
(body's clean-up
system)
Pain relieved
with movement
Legend: ↑ Blood flow carries heat to
affected joint tissues
Edema
(swelling)
Warmth
Erythema
(redness)
Fluid gradually builds in the
synovial membrane overnight
Morning joint stiffness
Lymphatic vessels
(body's clean-up system)
need ↑ time to reabsorb
↑ fluid that accumulated
overnight
Joint stiffness resolves ~1
hour after waking
Fragments of articular
(joint) cartilage trigger a
synovial (thin lining inside
of joints) inflammation
Inflammation causes fluid
to seep into the synovial
membrane during inactivity
Joints stiffen with rest
Moving the joint
physically pushes
inflammatory fluid back
into lymphatic vessels
(body's clean-up
system)
Joint stiffness resolves
within minutes of
movement
Pathophysiology Mechanism
Sign/Symptom/Lab Finding Complications
Published on www.thecalgaryguide.com
JOINT DISEASE: Inflammatory vs. Degenerative
Inflammatory Joint Disease
The body’s immune system fails to discriminate between self and non-self
Auto-immune cells attack body tissues
↑ Synovial (thin lining inside of the joint)
inflammation dilates blood vessels
↑ Endothelium (inner lining of blood
vessels) permeability
Synovial fluid accumulates &
leads to joint edema (swelling)
↑ Blood flow carries
heat to affected joint
tissues
Swelling activates
pain-sensitive joint
nociceptors
(damage alarms)
Fluid accumulates
progressively in the
synovial membrane
overnight
Edema
(swelling)
Warmth
Inflammatory pain
worse with rest
Morning joint
stiffness
Erythema
(redness)
Joint movement physically
pushes fluid back into
lymphatic vessels (body's
clean-up system)
Lymphatic vessels (body's
clean-up system) need ↑
time to reabsorb the ↑ fluid
that accumulated overnight
Inflammatory pain relieved
with activity
Joint stiffness resolves > 1hr
after waking
Legend: Mechanism
Sign/Symptom/Lab Finding Systemic
immune
activation occurs
↑
Inflammatory
mediators
circulate
throughout the
body
Extra-
articular
involvement
(e.g., skin,
eyes, lung,
heart,
kidneys) ±
abnormal
inflammatory
markers (CRP,
ESR) &
autoantibodi
es (RF, ANA)
Pathophysiology Complications
Degenerative Joint Disease
Abnormal mechanics or repetitive/excessive
loading stresses the joints
Joint structures degrade over time
Movement
(using the
joint)
exacerbates
the
mechanical
forces that are
wearing down
the joint
Pain with
movement
Pain relieved
with rest
Fragments of broken
articular cartilage
triggers a mild
synovial (thin lining
inside of the joint)
inflammation that
seeps fluid into the
synovial membrane
during inactivity
Joints stiffen with rest
Moving the joint
physically pushes
inflammatory fluid
back into lymphatic
vessels (body's clean-
up system) within
minutes
Joint stiffness resolves
within minutes of
movement
Published on www.thecalgaryguide.com
Authors:
Yan Yu
Mackenzie Trpcic
Reviewers:
Jennifer Au
Sean Spence
Martin Atkinson*
Catherine R Jarvis
* MD at time of
publication
The weight-
bearing joints
(i.e., knee, hip, &
lumbar/cervical
facet joints)
sustain the
highest
mechanical load
& degeneration
Distinguishing between Inflammatory and Degenerative joint disease
Inflammatory Joint
Disease
Auto-immune attack of body tissues, due to
failure of the body’s immune system to
discriminate between self and non-self.
Degenerative Joint
Disease
Repetitive, excess, or abnormal mechanical
forces on joints over time, leading to physical
breakdown of the joint.
Authors:
Yan Yu
Reviewers:
Jennifer Au
Sean Spence
Martin Atkinson*
* MD at time of
publication
Within joints, severe synovial inflammation
dilates local blood vessels, and causes the
vessel endothelium to be more leaky.
Accumulation of abundant
inflammatory synovial fluid
at rest or overnight
Swelling stimulates
joint nociceptors
Pain with rest
Moving the joint
physically pushes fluid
back into lymphatics,
relieving the painful
swelling.
Pain relieved with
motion
Legend: Overnight fluid
accumulation in the
synovial membrane
Morning stiffness
Lots of fluid, takes
more time (hours)
to be reabsorbed
by lymphatics
Stiffness resolves
after >1hr
Blood carries
heat and
looks red
Warm, Red,
Swollen
Joints
Pathophysiology Mechanism
Sign/Symptom/Lab Finding Inflammation is
oftentimes
systemic, not
localized
exclusively within
the joint (i.e. in
Rheumatoid
arthritis, Lupus,
etc)
Extra-articular
manifestations;
positive
inflammatory
markers (CRP,
ESR, RF, ANA)
Motion (using
the joint)
exacerbates the
mechanical
forces that are
wearing down
the joint
Fragments of
broken articular
cartilage triggers a
mild synovial
inflammation that
seeps fluid into the
synovial membrane
during inactivity
Pain with motion
(relieved by rest)
Joint stiffness
after inactivity
Moving the joint physically
pushes inflammatory fluid
back into lymphatics within
minutes.
Note: one big difference btw
the two is the degree of joint
inflammation (synovitis)
present in the joint capsule
Stiffness is short-lived,
quickly relieved by
movement
Published November1,2012 on www.thecalgaryguide.com
Larger, weight-
bearing joints tend to
bear the brunt of the
mechanical forces
Most commonly
affects the knee,
hip, and L/C-spine
facet joints
Complications" />
1hr
after waking
Legend: Mechanism
Sign/Symptom/Lab Finding Systemic
immune
activation occurs
↑
Inflammatory
mediators
circulate
throughout the
body
Extra-
articular
involvement
(e.g., skin,
eyes, lung,
heart,
kidneys) ±
abnormal
inflammatory
markers (CRP,
ESR) &
autoantibodi
es (RF, ANA)
Pathophysiology Complications
Degenerative Joint Disease
Abnormal mechanics or repetitive/excessive
loading stresses the joints
Joint structures degrade over time
Movement
(using the
joint)
exacerbates
the
mechanical
forces that are
wearing down
the joint
Pain with
movement
Pain relieved
with rest
Fragments of broken
articular cartilage
triggers a mild
synovial (thin lining
inside of the joint)
inflammation that
seeps fluid into the
synovial membrane
during inactivity
Joints stiffen with rest
Moving the joint
physically pushes
inflammatory fluid
back into lymphatic
vessels (body's clean-
up system) within
minutes
Joint stiffness resolves
within minutes of
movement
Published on www.thecalgaryguide.com
Authors:
Yan Yu
Mackenzie Trpcic
Reviewers:
Jennifer Au
Sean Spence
Martin Atkinson*
Catherine R Jarvis
* MD at time of
publication
The weight-
bearing joints
(i.e., knee, hip, &
lumbar/cervical
facet joints)
sustain the
highest
mechanical load
& degeneration
Distinguishing between Inflammatory and Degenerative joint disease
Inflammatory Joint
Disease
Auto-immune attack of body tissues, due to
failure of the body’s immune system to
discriminate between self and non-self.
Degenerative Joint
Disease
Repetitive, excess, or abnormal mechanical
forces on joints over time, leading to physical
breakdown of the joint.
Authors:
Yan Yu
Reviewers:
Jennifer Au
Sean Spence
Martin Atkinson*
* MD at time of
publication
Within joints, severe synovial inflammation
dilates local blood vessels, and causes the
vessel endothelium to be more leaky.
Accumulation of abundant
inflammatory synovial fluid
at rest or overnight
Swelling stimulates
joint nociceptors
Pain with rest
Moving the joint
physically pushes fluid
back into lymphatics,
relieving the painful
swelling.
Pain relieved with
motion
Legend: Overnight fluid
accumulation in the
synovial membrane
Morning stiffness
Lots of fluid, takes
more time (hours)
to be reabsorbed
by lymphatics
Stiffness resolves
after >1hr
Blood carries
heat and
looks red
Warm, Red,
Swollen
Joints
Pathophysiology Mechanism
Sign/Symptom/Lab Finding Inflammation is
oftentimes
systemic, not
localized
exclusively within
the joint (i.e. in
Rheumatoid
arthritis, Lupus,
etc)
Extra-articular
manifestations;
positive
inflammatory
markers (CRP,
ESR, RF, ANA)
Motion (using
the joint)
exacerbates the
mechanical
forces that are
wearing down
the joint
Fragments of
broken articular
cartilage triggers a
mild synovial
inflammation that
seeps fluid into the
synovial membrane
during inactivity
Pain with motion
(relieved by rest)
Joint stiffness
after inactivity
Moving the joint physically
pushes inflammatory fluid
back into lymphatics within
minutes.
Note: one big difference btw
the two is the degree of joint
inflammation (synovitis)
present in the joint capsule
Stiffness is short-lived,
quickly relieved by
movement
Published November1,2012 on www.thecalgaryguide.com
Larger, weight-
bearing joints tend to
bear the brunt of the
mechanical forces
Most commonly
affects the knee,
hip, and L/C-spine
facet joints
Complications" title="Legend: Inflammatory vs Degenerative Joint Disease: Pathogenesis & clinical findings
Inflammatory Joint Disease
The body’s immune system fails to discriminate between self & non-self
Autoimmune cells attack body tissues
↑ Synovial (thin lining inside of joints) inflammation
↑ Inflammation dilates blood vessels & activates the
endothelium (lining of blood vessels)
↑ Intercellular junctions open à "leaky" blood vessels
Synovial fluid
accumulates &
causes joint
edema (swelling)
↑ Blood flow
carries heat to
affected joint
tissues
Edema
(swelling)
Warmth
Erythema
(redness)
Fluid builds in
the synovial
membrane
overnight
Morning
joint
stiffness
Swelling
activates joint
nociceptors
(damage
alarms)
Pain worse
with rest
Systemic immune
activation occurs ↑ Inflammatory mediators
circulate throughout the body
Extra-
articular
(body tissues
outside of
joints)
inflammatory
damage
± ↑
Inflammatory
markers (CRP,
ESR)
± ↑ Auto-
antibodies
(RF, ANA)
Lymphatic vessels (the
body’s cleaning system)
need ↑ time to
reabsorb ↑ fluid that
accumulated overnight
Joint stiffness
resolves ~1 hour
after waking
Movement (using the
joint) pushes fluid into
lymphatic vessels (the
body’s cleaning system)
Pain relieved
with movement
Degenerative Joint Disease
Abnormal mechanics
(e.g., poor posture, weak
stabilizing muscles)
Repetitive or
excess stress on
joints
Weight bearing joints (knee, hip &
lumbar/cervical facet joints)
sustain the highest mechanical
load & degenerate over time
Fragments of articular
(joint) cartilage trigger a
synovial (thin lining inside
of joints) inflammation
Movement (using the
joint) exacerbates the
mechanical forces
wearing down the joint
Inflammation causes
fluid to seep into the
synovial membrane
during inactivity
Pain with
movement
Pain relieved
with rest
Joints stiffen with rest
Movement (using
the joint) pushes
fluid back into
lymphatic vessels
(the body’s
cleaning system)
Joint stiffness resolves
within minutes of
movement
Authors:
Yan Yu
Mackenzie Trpcic
Reviewers:
Jennifer Au
Sean Spence
Catherine R Jarvis
Martin Atkinson*
Glen Hazlewood*
* MD at time of publication
Published Nov 1, 2012; updated Feb 1, 2026 on www.thecalgaryguide.com
Pathophysiology Mechanism
Sign/Symptom/Lab Finding Complications
Final slide is the 1st slide
Legend: Inflammatory vs Degenerative Joint Disease: Pathogenesis & clinical findings
Inflammatory Joint Disease
Degenerative Joint Disease
The body’s immune system fails to discriminate between self & non-self
Autoimmune cells attack body tissues
Abnormal mechanics
(e.g., poor posture, weak
stabilizing muscles)
Repetitive or
excess stress on
joints
↑ Synovial (thin lining inside of joints)
inflammation dilates blood vessels
Systemic immune
activation occurs ↑ Endothelium (lining of blood vessels) activation
opens intercellular junctions (“leaky” blood vessels”)
↑ Inflammatory mediators
circulate throughout the body
Weight bearing joints (knee, hip &
lumbar/cervical facet joints)
sustain the highest mechanical
load & degenerate over time
Synovial fluid
accumulates &
causes joint
edema (swelling)
Edema
(swelling)
↑ Blood flow
carries heat to
affected joint
tissues
Extra-
articular
(body tissues
outside of
± ↑
Inflammatory
markers (CRP,
ESR)
± ↑ Auto-
antibodies
(RF, ANA)
Fragments of articular
(joint) cartilage trigger a
synovial (thin lining inside
of joints) inflammation
Movement (using the
joint) exacerbates the
mechanical forces
wearing down the joint
joints)
inflammatory
Inflammation causes
Warmth Pain relieved
Erythema
damage
fluid to seep into the
Pain with
(redness)
synovial membrane
movement
with rest
during inactivity
Fluid builds in
the synovial
membrane
overnight
Morning
joint
stiffness
Lymphatic
vessels (cleaners)
need ↑ time to
reabsorb ↑ fluid
that accumulated
overnight
Joints stiffen
with rest
Joint stiffness resolves
~1 hour after waking
Movement (using
the joint) pushes
fluid back into
lymphatic vessels
(cleaners)
Swelling
activates joint
nociceptors
(damage
alarms)
Pain worse
with rest
Movement (using
the joint) pushes
fluid into
lymphatic vessels
(cleaners)
Pain relieved with
movement
Joint stiffness
resolves within
minutes of
movement
Authors:
Yan Yu
Mackenzie Trpcic
Reviewers:
Jennifer Au
Sean Spence
Martin Atkinson*
Catherine R Jarvis
* MD at time of
publication
Published on www.thecalgaryguide.com
Pathophysiology Mechanism
Sign/Symptom/Lab Finding Complications
Inflammatory vs Degenerative Joint Disease: Pathogenesis & clinical findings
Inflammatory Joint Disease
Degenerative Joint Disease
The body’s immune system fails to discriminate between self & non-self
Auto-immune cells attack body tissues
Abnormal mechanics
(e.g., poor posture, weak
stabilizing muscles)
Repetitive or
excess stress on
joints
↑ Synovial (thin lining inside of joints)
inflammation dilates blood vessels
Systemic immune
activation occurs ↑ Endothelium (lining of blood vessels) activation
opens intercellular junctions (“leaky” blood vessels”)
↑ Inflammatory mediators
circulate throughout the body
Weight bearing joints (knee, hip &
lumbar/cervical facet joints)
sustain the highest mechanical
load & degenerate over time
Synovial fluid accumulates &
leads to joint edema (swelling)
↑ Blood flow carries heat
to affected joint tissues
Swelling
activates
joint
nociceptors
(damage
alarms)
Fluid
builds in
the
synovial
membrane
overnight
Edema
(swelling)
Warmth
Erythema
(redness)
Extra-articular
(body tissues
outside of
joints)
inflammatory
damage
± ↑
Inflammatory
markers (CRP,
ESR) & auto-
antibodies
(RF, ANA)
Movement (using the
joint) exacerbates the
mechanical forces
wearing down the joint
Pain with
movement
Pain relieved
with rest
Pain worse
with rest
Morning
joint stiffness
Movement
(using the
joint) pushes
fluid into
lymphatic
vessels
(cleaners)
Lymphatic
vessels
(cleaners)
need ↑ time
to reabsorb
↑ fluid
overnight
Pain relieved
with
movement
Joint stiffness
resolves ~1 hour
after waking
Authors:
Yan Yu
Mackenzie Trpcic
Reviewers:
Jennifer Au
Sean Spence
Martin Atkinson*
Catherine R Jarvis
* MD at time of
publication
Legend: Pathophysiology Mechanism
Sign/Symptom/Lab Finding Complications
Fragments of articular
(joint) cartilage trigger a
synovial (thin lining inside
of joints) inflammation
Inflammation causes
fluid to seep into the
synovial membrane
during inactivity
Joints stiffen
with rest
Movement (using
the joint) pushes
inflammatory fluid
back into lymphatic
vessels (cleaners)
Joint stiffness
resolves within
minutes of
movement
Published on www.thecalgaryguide.com
Inflammatory vs Degenerative Joint Disease: Pathogenesis & clinical findings
Inflammatory Joint Disease
The body’s immune system fails to discriminate between self and non-self
Auto-immune cells attack body tissues
↑ Synovial (thin lining inside of joints)
inflammation dilates blood vessels
↑ Endothelium (lining inside of
blood vessels) permeability
Synovial fluid accumulates &
leads to joint edema
(swelling)
Systemic immune
activation occurs
↑ Inflammatory mediators
circulate throughout the
body
Extra-articular
involvement
(body tissues
outside of
joints)
Elevated
inflammatory
markers (CRP,
ESR) & auto-
antibodies
(RF, ANA)
Degenerative Joint Disease
Abnormal
mechanics (e.g.,
poor posture,
weak stabilizing
muscles)
Repetitive/excess
stress on joints
Weight bearing joints (knee, hip &
lumbar/cervical facet joints)
sustain the highest mechanical
load & degenerate over time
Movement (using the joint)
exacerbates the mechanical
forces wearing down the
joint
Pain with
movement
Pain
relieved
with
rest
Authors:
Yan Yu
Mackenzie Trpcic
Reviewers:
Jennifer Au
Sean Spence
Martin Atkinson*
Catherine R Jarvis
* MD at time of
publication
Swelling activates
pain-sensitive joint
nociceptors
(damage alarms)
Pain worse with rest
Joint movement
pushes fluid into
lymphatic vessels
(body's clean-up
system)
Pain relieved
with movement
Legend: ↑ Blood flow carries heat to
affected joint tissues
Edema
(swelling)
Warmth
Erythema
(redness)
Fluid gradually builds in the
synovial membrane overnight
Morning joint stiffness
Lymphatic vessels
(body's clean-up system)
need ↑ time to reabsorb
↑ fluid that accumulated
overnight
Joint stiffness resolves ~1
hour after waking
Fragments of articular
(joint) cartilage trigger a
synovial (thin lining inside
of joints) inflammation
Inflammation causes fluid
to seep into the synovial
membrane during inactivity
Joints stiffen with rest
Moving the joint
physically pushes
inflammatory fluid back
into lymphatic vessels
(body's clean-up
system)
Joint stiffness resolves
within minutes of
movement
Pathophysiology Mechanism
Sign/Symptom/Lab Finding Complications
Published on www.thecalgaryguide.com
JOINT DISEASE: Inflammatory vs. Degenerative
Inflammatory Joint Disease
The body’s immune system fails to discriminate between self and non-self
Auto-immune cells attack body tissues
↑ Synovial (thin lining inside of the joint)
inflammation dilates blood vessels
↑ Endothelium (inner lining of blood
vessels) permeability
Synovial fluid accumulates &
leads to joint edema (swelling)
↑ Blood flow carries
heat to affected joint
tissues
Swelling activates
pain-sensitive joint
nociceptors
(damage alarms)
Fluid accumulates
progressively in the
synovial membrane
overnight
Edema
(swelling)
Warmth
Inflammatory pain
worse with rest
Morning joint
stiffness
Erythema
(redness)
Joint movement physically
pushes fluid back into
lymphatic vessels (body's
clean-up system)
Lymphatic vessels (body's
clean-up system) need ↑
time to reabsorb the ↑ fluid
that accumulated overnight
Inflammatory pain relieved
with activity
Joint stiffness resolves > 1hr
after waking
Legend: Mechanism
Sign/Symptom/Lab Finding Systemic
immune
activation occurs
↑
Inflammatory
mediators
circulate
throughout the
body
Extra-
articular
involvement
(e.g., skin,
eyes, lung,
heart,
kidneys) ±
abnormal
inflammatory
markers (CRP,
ESR) &
autoantibodi
es (RF, ANA)
Pathophysiology Complications
Degenerative Joint Disease
Abnormal mechanics or repetitive/excessive
loading stresses the joints
Joint structures degrade over time
Movement
(using the
joint)
exacerbates
the
mechanical
forces that are
wearing down
the joint
Pain with
movement
Pain relieved
with rest
Fragments of broken
articular cartilage
triggers a mild
synovial (thin lining
inside of the joint)
inflammation that
seeps fluid into the
synovial membrane
during inactivity
Joints stiffen with rest
Moving the joint
physically pushes
inflammatory fluid
back into lymphatic
vessels (body's clean-
up system) within
minutes
Joint stiffness resolves
within minutes of
movement
Published on www.thecalgaryguide.com
Authors:
Yan Yu
Mackenzie Trpcic
Reviewers:
Jennifer Au
Sean Spence
Martin Atkinson*
Catherine R Jarvis
* MD at time of
publication
The weight-
bearing joints
(i.e., knee, hip, &
lumbar/cervical
facet joints)
sustain the
highest
mechanical load
& degeneration
Distinguishing between Inflammatory and Degenerative joint disease
Inflammatory Joint
Disease
Auto-immune attack of body tissues, due to
failure of the body’s immune system to
discriminate between self and non-self.
Degenerative Joint
Disease
Repetitive, excess, or abnormal mechanical
forces on joints over time, leading to physical
breakdown of the joint.
Authors:
Yan Yu
Reviewers:
Jennifer Au
Sean Spence
Martin Atkinson*
* MD at time of
publication
Within joints, severe synovial inflammation
dilates local blood vessels, and causes the
vessel endothelium to be more leaky.
Accumulation of abundant
inflammatory synovial fluid
at rest or overnight
Swelling stimulates
joint nociceptors
Pain with rest
Moving the joint
physically pushes fluid
back into lymphatics,
relieving the painful
swelling.
Pain relieved with
motion
Legend: Overnight fluid
accumulation in the
synovial membrane
Morning stiffness
Lots of fluid, takes
more time (hours)
to be reabsorbed
by lymphatics
Stiffness resolves
after >1hr
Blood carries
heat and
looks red
Warm, Red,
Swollen
Joints
Pathophysiology Mechanism
Sign/Symptom/Lab Finding Inflammation is
oftentimes
systemic, not
localized
exclusively within
the joint (i.e. in
Rheumatoid
arthritis, Lupus,
etc)
Extra-articular
manifestations;
positive
inflammatory
markers (CRP,
ESR, RF, ANA)
Motion (using
the joint)
exacerbates the
mechanical
forces that are
wearing down
the joint
Fragments of
broken articular
cartilage triggers a
mild synovial
inflammation that
seeps fluid into the
synovial membrane
during inactivity
Pain with motion
(relieved by rest)
Joint stiffness
after inactivity
Moving the joint physically
pushes inflammatory fluid
back into lymphatics within
minutes.
Note: one big difference btw
the two is the degree of joint
inflammation (synovitis)
present in the joint capsule
Stiffness is short-lived,
quickly relieved by
movement
Published November1,2012 on www.thecalgaryguide.com
Larger, weight-
bearing joints tend to
bear the brunt of the
mechanical forces
Most commonly
affects the knee,
hip, and L/C-spine
facet joints
Complications" />
 1hr
after waking
Legend: Mechanism
Sign/Symptom/Lab Finding Systemic
immune
activation occurs
↑
Inflammatory
mediators
circulate
throughout the
body
Extra-
articular
involvement
(e.g., skin,
eyes, lung,
heart,
kidneys) ±
abnormal
inflammatory
markers (CRP,
ESR) &
autoantibodi
es (RF, ANA)
Pathophysiology Complications
Degenerative Joint Disease
Abnormal mechanics or repetitive/excessive
loading stresses the joints
Joint structures degrade over time
Movement
(using the
joint)
exacerbates
the
mechanical
forces that are
wearing down
the joint
Pain with
movement
Pain relieved
with rest
Fragments of broken
articular cartilage
triggers a mild
synovial (thin lining
inside of the joint)
inflammation that
seeps fluid into the
synovial membrane
during inactivity
Joints stiffen with rest
Moving the joint
physically pushes
inflammatory fluid
back into lymphatic
vessels (body's clean-
up system) within
minutes
Joint stiffness resolves
within minutes of
movement
Published on www.thecalgaryguide.com
Authors:
Yan Yu
Mackenzie Trpcic
Reviewers:
Jennifer Au
Sean Spence
Martin Atkinson*
Catherine R Jarvis
* MD at time of
publication
The weight-
bearing joints
(i.e., knee, hip, &
lumbar/cervical
facet joints)
sustain the
highest
mechanical load
& degeneration
Distinguishing between Inflammatory and Degenerative joint disease
Inflammatory Joint
Disease
Auto-immune attack of body tissues, due to
failure of the body’s immune system to
discriminate between self and non-self.
Degenerative Joint
Disease
Repetitive, excess, or abnormal mechanical
forces on joints over time, leading to physical
breakdown of the joint.
Authors:
Yan Yu
Reviewers:
Jennifer Au
Sean Spence
Martin Atkinson*
* MD at time of
publication
Within joints, severe synovial inflammation
dilates local blood vessels, and causes the
vessel endothelium to be more leaky.
Accumulation of abundant
inflammatory synovial fluid
at rest or overnight
Swelling stimulates
joint nociceptors
Pain with rest
Moving the joint
physically pushes fluid
back into lymphatics,
relieving the painful
swelling.
Pain relieved with
motion
Legend: Overnight fluid
accumulation in the
synovial membrane
Morning stiffness
Lots of fluid, takes
more time (hours)
to be reabsorbed
by lymphatics
Stiffness resolves
after >1hr
Blood carries
heat and
looks red
Warm, Red,
Swollen
Joints
Pathophysiology Mechanism
Sign/Symptom/Lab Finding Inflammation is
oftentimes
systemic, not
localized
exclusively within
the joint (i.e. in
Rheumatoid
arthritis, Lupus,
etc)
Extra-articular
manifestations;
positive
inflammatory
markers (CRP,
ESR, RF, ANA)
Motion (using
the joint)
exacerbates the
mechanical
forces that are
wearing down
the joint
Fragments of
broken articular
cartilage triggers a
mild synovial
inflammation that
seeps fluid into the
synovial membrane
during inactivity
Pain with motion
(relieved by rest)
Joint stiffness
after inactivity
Moving the joint physically
pushes inflammatory fluid
back into lymphatics within
minutes.
Note: one big difference btw
the two is the degree of joint
inflammation (synovitis)
present in the joint capsule
Stiffness is short-lived,
quickly relieved by
movement
Published November1,2012 on www.thecalgaryguide.com
Larger, weight-
bearing joints tend to
bear the brunt of the
mechanical forces
Most commonly
affects the knee,
hip, and L/C-spine
facet joints
Complications" title="Legend: Inflammatory vs Degenerative Joint Disease: Pathogenesis & clinical findings
Inflammatory Joint Disease
The body’s immune system fails to discriminate between self & non-self
Autoimmune cells attack body tissues
↑ Synovial (thin lining inside of joints) inflammation
↑ Inflammation dilates blood vessels & activates the
endothelium (lining of blood vessels)
↑ Intercellular junctions open à "leaky" blood vessels
Synovial fluid
accumulates &
causes joint
edema (swelling)
↑ Blood flow
carries heat to
affected joint
tissues
Edema
(swelling)
Warmth
Erythema
(redness)
Fluid builds in
the synovial
membrane
overnight
Morning
joint
stiffness
Swelling
activates joint
nociceptors
(damage
alarms)
Pain worse
with rest
Systemic immune
activation occurs ↑ Inflammatory mediators
circulate throughout the body
Extra-
articular
(body tissues
outside of
joints)
inflammatory
damage
± ↑
Inflammatory
markers (CRP,
ESR)
± ↑ Auto-
antibodies
(RF, ANA)
Lymphatic vessels (the
body’s cleaning system)
need ↑ time to
reabsorb ↑ fluid that
accumulated overnight
Joint stiffness
resolves ~1 hour
after waking
Movement (using the
joint) pushes fluid into
lymphatic vessels (the
body’s cleaning system)
Pain relieved
with movement
Degenerative Joint Disease
Abnormal mechanics
(e.g., poor posture, weak
stabilizing muscles)
Repetitive or
excess stress on
joints
Weight bearing joints (knee, hip &
lumbar/cervical facet joints)
sustain the highest mechanical
load & degenerate over time
Fragments of articular
(joint) cartilage trigger a
synovial (thin lining inside
of joints) inflammation
Movement (using the
joint) exacerbates the
mechanical forces
wearing down the joint
Inflammation causes
fluid to seep into the
synovial membrane
during inactivity
Pain with
movement
Pain relieved
with rest
Joints stiffen with rest
Movement (using
the joint) pushes
fluid back into
lymphatic vessels
(the body’s
cleaning system)
Joint stiffness resolves
within minutes of
movement
Authors:
Yan Yu
Mackenzie Trpcic
Reviewers:
Jennifer Au
Sean Spence
Catherine R Jarvis
Martin Atkinson*
Glen Hazlewood*
* MD at time of publication
Published Nov 1, 2012; updated Feb 1, 2026 on www.thecalgaryguide.com
Pathophysiology Mechanism
Sign/Symptom/Lab Finding Complications
Final slide is the 1st slide
Legend: Inflammatory vs Degenerative Joint Disease: Pathogenesis & clinical findings
Inflammatory Joint Disease
Degenerative Joint Disease
The body’s immune system fails to discriminate between self & non-self
Autoimmune cells attack body tissues
Abnormal mechanics
(e.g., poor posture, weak
stabilizing muscles)
Repetitive or
excess stress on
joints
↑ Synovial (thin lining inside of joints)
inflammation dilates blood vessels
Systemic immune
activation occurs ↑ Endothelium (lining of blood vessels) activation
opens intercellular junctions (“leaky” blood vessels”)
↑ Inflammatory mediators
circulate throughout the body
Weight bearing joints (knee, hip &
lumbar/cervical facet joints)
sustain the highest mechanical
load & degenerate over time
Synovial fluid
accumulates &
causes joint
edema (swelling)
Edema
(swelling)
↑ Blood flow
carries heat to
affected joint
tissues
Extra-
articular
(body tissues
outside of
± ↑
Inflammatory
markers (CRP,
ESR)
± ↑ Auto-
antibodies
(RF, ANA)
Fragments of articular
(joint) cartilage trigger a
synovial (thin lining inside
of joints) inflammation
Movement (using the
joint) exacerbates the
mechanical forces
wearing down the joint
joints)
inflammatory
Inflammation causes
Warmth Pain relieved
Erythema
damage
fluid to seep into the
Pain with
(redness)
synovial membrane
movement
with rest
during inactivity
Fluid builds in
the synovial
membrane
overnight
Morning
joint
stiffness
Lymphatic
vessels (cleaners)
need ↑ time to
reabsorb ↑ fluid
that accumulated
overnight
Joints stiffen
with rest
Joint stiffness resolves
~1 hour after waking
Movement (using
the joint) pushes
fluid back into
lymphatic vessels
(cleaners)
Swelling
activates joint
nociceptors
(damage
alarms)
Pain worse
with rest
Movement (using
the joint) pushes
fluid into
lymphatic vessels
(cleaners)
Pain relieved with
movement
Joint stiffness
resolves within
minutes of
movement
Authors:
Yan Yu
Mackenzie Trpcic
Reviewers:
Jennifer Au
Sean Spence
Martin Atkinson*
Catherine R Jarvis
* MD at time of
publication
Published on www.thecalgaryguide.com
Pathophysiology Mechanism
Sign/Symptom/Lab Finding Complications
Inflammatory vs Degenerative Joint Disease: Pathogenesis & clinical findings
Inflammatory Joint Disease
Degenerative Joint Disease
The body’s immune system fails to discriminate between self & non-self
Auto-immune cells attack body tissues
Abnormal mechanics
(e.g., poor posture, weak
stabilizing muscles)
Repetitive or
excess stress on
joints
↑ Synovial (thin lining inside of joints)
inflammation dilates blood vessels
Systemic immune
activation occurs ↑ Endothelium (lining of blood vessels) activation
opens intercellular junctions (“leaky” blood vessels”)
↑ Inflammatory mediators
circulate throughout the body
Weight bearing joints (knee, hip &
lumbar/cervical facet joints)
sustain the highest mechanical
load & degenerate over time
Synovial fluid accumulates &
leads to joint edema (swelling)
↑ Blood flow carries heat
to affected joint tissues
Swelling
activates
joint
nociceptors
(damage
alarms)
Fluid
builds in
the
synovial
membrane
overnight
Edema
(swelling)
Warmth
Erythema
(redness)
Extra-articular
(body tissues
outside of
joints)
inflammatory
damage
± ↑
Inflammatory
markers (CRP,
ESR) & auto-
antibodies
(RF, ANA)
Movement (using the
joint) exacerbates the
mechanical forces
wearing down the joint
Pain with
movement
Pain relieved
with rest
Pain worse
with rest
Morning
joint stiffness
Movement
(using the
joint) pushes
fluid into
lymphatic
vessels
(cleaners)
Lymphatic
vessels
(cleaners)
need ↑ time
to reabsorb
↑ fluid
overnight
Pain relieved
with
movement
Joint stiffness
resolves ~1 hour
after waking
Authors:
Yan Yu
Mackenzie Trpcic
Reviewers:
Jennifer Au
Sean Spence
Martin Atkinson*
Catherine R Jarvis
* MD at time of
publication
Legend: Pathophysiology Mechanism
Sign/Symptom/Lab Finding Complications
Fragments of articular
(joint) cartilage trigger a
synovial (thin lining inside
of joints) inflammation
Inflammation causes
fluid to seep into the
synovial membrane
during inactivity
Joints stiffen
with rest
Movement (using
the joint) pushes
inflammatory fluid
back into lymphatic
vessels (cleaners)
Joint stiffness
resolves within
minutes of
movement
Published on www.thecalgaryguide.com
Inflammatory vs Degenerative Joint Disease: Pathogenesis & clinical findings
Inflammatory Joint Disease
The body’s immune system fails to discriminate between self and non-self
Auto-immune cells attack body tissues
↑ Synovial (thin lining inside of joints)
inflammation dilates blood vessels
↑ Endothelium (lining inside of
blood vessels) permeability
Synovial fluid accumulates &
leads to joint edema
(swelling)
Systemic immune
activation occurs
↑ Inflammatory mediators
circulate throughout the
body
Extra-articular
involvement
(body tissues
outside of
joints)
Elevated
inflammatory
markers (CRP,
ESR) & auto-
antibodies
(RF, ANA)
Degenerative Joint Disease
Abnormal
mechanics (e.g.,
poor posture,
weak stabilizing
muscles)
Repetitive/excess
stress on joints
Weight bearing joints (knee, hip &
lumbar/cervical facet joints)
sustain the highest mechanical
load & degenerate over time
Movement (using the joint)
exacerbates the mechanical
forces wearing down the
joint
Pain with
movement
Pain
relieved
with
rest
Authors:
Yan Yu
Mackenzie Trpcic
Reviewers:
Jennifer Au
Sean Spence
Martin Atkinson*
Catherine R Jarvis
* MD at time of
publication
Swelling activates
pain-sensitive joint
nociceptors
(damage alarms)
Pain worse with rest
Joint movement
pushes fluid into
lymphatic vessels
(body's clean-up
system)
Pain relieved
with movement
Legend: ↑ Blood flow carries heat to
affected joint tissues
Edema
(swelling)
Warmth
Erythema
(redness)
Fluid gradually builds in the
synovial membrane overnight
Morning joint stiffness
Lymphatic vessels
(body's clean-up system)
need ↑ time to reabsorb
↑ fluid that accumulated
overnight
Joint stiffness resolves ~1
hour after waking
Fragments of articular
(joint) cartilage trigger a
synovial (thin lining inside
of joints) inflammation
Inflammation causes fluid
to seep into the synovial
membrane during inactivity
Joints stiffen with rest
Moving the joint
physically pushes
inflammatory fluid back
into lymphatic vessels
(body's clean-up
system)
Joint stiffness resolves
within minutes of
movement
Pathophysiology Mechanism
Sign/Symptom/Lab Finding Complications
Published on www.thecalgaryguide.com
JOINT DISEASE: Inflammatory vs. Degenerative
Inflammatory Joint Disease
The body’s immune system fails to discriminate between self and non-self
Auto-immune cells attack body tissues
↑ Synovial (thin lining inside of the joint)
inflammation dilates blood vessels
↑ Endothelium (inner lining of blood
vessels) permeability
Synovial fluid accumulates &
leads to joint edema (swelling)
↑ Blood flow carries
heat to affected joint
tissues
Swelling activates
pain-sensitive joint
nociceptors
(damage alarms)
Fluid accumulates
progressively in the
synovial membrane
overnight
Edema
(swelling)
Warmth
Inflammatory pain
worse with rest
Morning joint
stiffness
Erythema
(redness)
Joint movement physically
pushes fluid back into
lymphatic vessels (body's
clean-up system)
Lymphatic vessels (body's
clean-up system) need ↑
time to reabsorb the ↑ fluid
that accumulated overnight
Inflammatory pain relieved
with activity
Joint stiffness resolves > 1hr
after waking
Legend: Mechanism
Sign/Symptom/Lab Finding Systemic
immune
activation occurs
↑
Inflammatory
mediators
circulate
throughout the
body
Extra-
articular
involvement
(e.g., skin,
eyes, lung,
heart,
kidneys) ±
abnormal
inflammatory
markers (CRP,
ESR) &
autoantibodi
es (RF, ANA)
Pathophysiology Complications
Degenerative Joint Disease
Abnormal mechanics or repetitive/excessive
loading stresses the joints
Joint structures degrade over time
Movement
(using the
joint)
exacerbates
the
mechanical
forces that are
wearing down
the joint
Pain with
movement
Pain relieved
with rest
Fragments of broken
articular cartilage
triggers a mild
synovial (thin lining
inside of the joint)
inflammation that
seeps fluid into the
synovial membrane
during inactivity
Joints stiffen with rest
Moving the joint
physically pushes
inflammatory fluid
back into lymphatic
vessels (body's clean-
up system) within
minutes
Joint stiffness resolves
within minutes of
movement
Published on www.thecalgaryguide.com
Authors:
Yan Yu
Mackenzie Trpcic
Reviewers:
Jennifer Au
Sean Spence
Martin Atkinson*
Catherine R Jarvis
* MD at time of
publication
The weight-
bearing joints
(i.e., knee, hip, &
lumbar/cervical
facet joints)
sustain the
highest
mechanical load
& degeneration
Distinguishing between Inflammatory and Degenerative joint disease
Inflammatory Joint
Disease
Auto-immune attack of body tissues, due to
failure of the body’s immune system to
discriminate between self and non-self.
Degenerative Joint
Disease
Repetitive, excess, or abnormal mechanical
forces on joints over time, leading to physical
breakdown of the joint.
Authors:
Yan Yu
Reviewers:
Jennifer Au
Sean Spence
Martin Atkinson*
* MD at time of
publication
Within joints, severe synovial inflammation
dilates local blood vessels, and causes the
vessel endothelium to be more leaky.
Accumulation of abundant
inflammatory synovial fluid
at rest or overnight
Swelling stimulates
joint nociceptors
Pain with rest
Moving the joint
physically pushes fluid
back into lymphatics,
relieving the painful
swelling.
Pain relieved with
motion
Legend: Overnight fluid
accumulation in the
synovial membrane
Morning stiffness
Lots of fluid, takes
more time (hours)
to be reabsorbed
by lymphatics
Stiffness resolves
after >1hr
Blood carries
heat and
looks red
Warm, Red,
Swollen
Joints
Pathophysiology Mechanism
Sign/Symptom/Lab Finding Inflammation is
oftentimes
systemic, not
localized
exclusively within
the joint (i.e. in
Rheumatoid
arthritis, Lupus,
etc)
Extra-articular
manifestations;
positive
inflammatory
markers (CRP,
ESR, RF, ANA)
Motion (using
the joint)
exacerbates the
mechanical
forces that are
wearing down
the joint
Fragments of
broken articular
cartilage triggers a
mild synovial
inflammation that
seeps fluid into the
synovial membrane
during inactivity
Pain with motion
(relieved by rest)
Joint stiffness
after inactivity
Moving the joint physically
pushes inflammatory fluid
back into lymphatics within
minutes.
Note: one big difference btw
the two is the degree of joint
inflammation (synovitis)
present in the joint capsule
Stiffness is short-lived,
quickly relieved by
movement
Published November1,2012 on www.thecalgaryguide.com
Larger, weight-
bearing joints tend to
bear the brunt of the
mechanical forces
Most commonly
affects the knee,
hip, and L/C-spine
facet joints
Complications" />
1hr
after waking
Legend: Mechanism
Sign/Symptom/Lab Finding Systemic
immune
activation occurs
↑
Inflammatory
mediators
circulate
throughout the
body
Extra-
articular
involvement
(e.g., skin,
eyes, lung,
heart,
kidneys) ±
abnormal
inflammatory
markers (CRP,
ESR) &
autoantibodi
es (RF, ANA)
Pathophysiology Complications
Degenerative Joint Disease
Abnormal mechanics or repetitive/excessive
loading stresses the joints
Joint structures degrade over time
Movement
(using the
joint)
exacerbates
the
mechanical
forces that are
wearing down
the joint
Pain with
movement
Pain relieved
with rest
Fragments of broken
articular cartilage
triggers a mild
synovial (thin lining
inside of the joint)
inflammation that
seeps fluid into the
synovial membrane
during inactivity
Joints stiffen with rest
Moving the joint
physically pushes
inflammatory fluid
back into lymphatic
vessels (body's clean-
up system) within
minutes
Joint stiffness resolves
within minutes of
movement
Published on www.thecalgaryguide.com
Authors:
Yan Yu
Mackenzie Trpcic
Reviewers:
Jennifer Au
Sean Spence
Martin Atkinson*
Catherine R Jarvis
* MD at time of
publication
The weight-
bearing joints
(i.e., knee, hip, &
lumbar/cervical
facet joints)
sustain the
highest
mechanical load
& degeneration
Distinguishing between Inflammatory and Degenerative joint disease
Inflammatory Joint
Disease
Auto-immune attack of body tissues, due to
failure of the body’s immune system to
discriminate between self and non-self.
Degenerative Joint
Disease
Repetitive, excess, or abnormal mechanical
forces on joints over time, leading to physical
breakdown of the joint.
Authors:
Yan Yu
Reviewers:
Jennifer Au
Sean Spence
Martin Atkinson*
* MD at time of
publication
Within joints, severe synovial inflammation
dilates local blood vessels, and causes the
vessel endothelium to be more leaky.
Accumulation of abundant
inflammatory synovial fluid
at rest or overnight
Swelling stimulates
joint nociceptors
Pain with rest
Moving the joint
physically pushes fluid
back into lymphatics,
relieving the painful
swelling.
Pain relieved with
motion
Legend: Overnight fluid
accumulation in the
synovial membrane
Morning stiffness
Lots of fluid, takes
more time (hours)
to be reabsorbed
by lymphatics
Stiffness resolves
after >1hr
Blood carries
heat and
looks red
Warm, Red,
Swollen
Joints
Pathophysiology Mechanism
Sign/Symptom/Lab Finding Inflammation is
oftentimes
systemic, not
localized
exclusively within
the joint (i.e. in
Rheumatoid
arthritis, Lupus,
etc)
Extra-articular
manifestations;
positive
inflammatory
markers (CRP,
ESR, RF, ANA)
Motion (using
the joint)
exacerbates the
mechanical
forces that are
wearing down
the joint
Fragments of
broken articular
cartilage triggers a
mild synovial
inflammation that
seeps fluid into the
synovial membrane
during inactivity
Pain with motion
(relieved by rest)
Joint stiffness
after inactivity
Moving the joint physically
pushes inflammatory fluid
back into lymphatics within
minutes.
Note: one big difference btw
the two is the degree of joint
inflammation (synovitis)
present in the joint capsule
Stiffness is short-lived,
quickly relieved by
movement
Published November1,2012 on www.thecalgaryguide.com
Larger, weight-
bearing joints tend to
bear the brunt of the
mechanical forces
Most commonly
affects the knee,
hip, and L/C-spine
facet joints
Complications" title="Legend: Inflammatory vs Degenerative Joint Disease: Pathogenesis & clinical findings
Inflammatory Joint Disease
The body’s immune system fails to discriminate between self & non-self
Autoimmune cells attack body tissues
↑ Synovial (thin lining inside of joints) inflammation
↑ Inflammation dilates blood vessels & activates the
endothelium (lining of blood vessels)
↑ Intercellular junctions open à "leaky" blood vessels
Synovial fluid
accumulates &
causes joint
edema (swelling)
↑ Blood flow
carries heat to
affected joint
tissues
Edema
(swelling)
Warmth
Erythema
(redness)
Fluid builds in
the synovial
membrane
overnight
Morning
joint
stiffness
Swelling
activates joint
nociceptors
(damage
alarms)
Pain worse
with rest
Systemic immune
activation occurs ↑ Inflammatory mediators
circulate throughout the body
Extra-
articular
(body tissues
outside of
joints)
inflammatory
damage
± ↑
Inflammatory
markers (CRP,
ESR)
± ↑ Auto-
antibodies
(RF, ANA)
Lymphatic vessels (the
body’s cleaning system)
need ↑ time to
reabsorb ↑ fluid that
accumulated overnight
Joint stiffness
resolves ~1 hour
after waking
Movement (using the
joint) pushes fluid into
lymphatic vessels (the
body’s cleaning system)
Pain relieved
with movement
Degenerative Joint Disease
Abnormal mechanics
(e.g., poor posture, weak
stabilizing muscles)
Repetitive or
excess stress on
joints
Weight bearing joints (knee, hip &
lumbar/cervical facet joints)
sustain the highest mechanical
load & degenerate over time
Fragments of articular
(joint) cartilage trigger a
synovial (thin lining inside
of joints) inflammation
Movement (using the
joint) exacerbates the
mechanical forces
wearing down the joint
Inflammation causes
fluid to seep into the
synovial membrane
during inactivity
Pain with
movement
Pain relieved
with rest
Joints stiffen with rest
Movement (using
the joint) pushes
fluid back into
lymphatic vessels
(the body’s
cleaning system)
Joint stiffness resolves
within minutes of
movement
Authors:
Yan Yu
Mackenzie Trpcic
Reviewers:
Jennifer Au
Sean Spence
Catherine R Jarvis
Martin Atkinson*
Glen Hazlewood*
* MD at time of publication
Published Nov 1, 2012; updated Feb 1, 2026 on www.thecalgaryguide.com
Pathophysiology Mechanism
Sign/Symptom/Lab Finding Complications
Final slide is the 1st slide
Legend: Inflammatory vs Degenerative Joint Disease: Pathogenesis & clinical findings
Inflammatory Joint Disease
Degenerative Joint Disease
The body’s immune system fails to discriminate between self & non-self
Autoimmune cells attack body tissues
Abnormal mechanics
(e.g., poor posture, weak
stabilizing muscles)
Repetitive or
excess stress on
joints
↑ Synovial (thin lining inside of joints)
inflammation dilates blood vessels
Systemic immune
activation occurs ↑ Endothelium (lining of blood vessels) activation
opens intercellular junctions (“leaky” blood vessels”)
↑ Inflammatory mediators
circulate throughout the body
Weight bearing joints (knee, hip &
lumbar/cervical facet joints)
sustain the highest mechanical
load & degenerate over time
Synovial fluid
accumulates &
causes joint
edema (swelling)
Edema
(swelling)
↑ Blood flow
carries heat to
affected joint
tissues
Extra-
articular
(body tissues
outside of
± ↑
Inflammatory
markers (CRP,
ESR)
± ↑ Auto-
antibodies
(RF, ANA)
Fragments of articular
(joint) cartilage trigger a
synovial (thin lining inside
of joints) inflammation
Movement (using the
joint) exacerbates the
mechanical forces
wearing down the joint
joints)
inflammatory
Inflammation causes
Warmth Pain relieved
Erythema
damage
fluid to seep into the
Pain with
(redness)
synovial membrane
movement
with rest
during inactivity
Fluid builds in
the synovial
membrane
overnight
Morning
joint
stiffness
Lymphatic
vessels (cleaners)
need ↑ time to
reabsorb ↑ fluid
that accumulated
overnight
Joints stiffen
with rest
Joint stiffness resolves
~1 hour after waking
Movement (using
the joint) pushes
fluid back into
lymphatic vessels
(cleaners)
Swelling
activates joint
nociceptors
(damage
alarms)
Pain worse
with rest
Movement (using
the joint) pushes
fluid into
lymphatic vessels
(cleaners)
Pain relieved with
movement
Joint stiffness
resolves within
minutes of
movement
Authors:
Yan Yu
Mackenzie Trpcic
Reviewers:
Jennifer Au
Sean Spence
Martin Atkinson*
Catherine R Jarvis
* MD at time of
publication
Published on www.thecalgaryguide.com
Pathophysiology Mechanism
Sign/Symptom/Lab Finding Complications
Inflammatory vs Degenerative Joint Disease: Pathogenesis & clinical findings
Inflammatory Joint Disease
Degenerative Joint Disease
The body’s immune system fails to discriminate between self & non-self
Auto-immune cells attack body tissues
Abnormal mechanics
(e.g., poor posture, weak
stabilizing muscles)
Repetitive or
excess stress on
joints
↑ Synovial (thin lining inside of joints)
inflammation dilates blood vessels
Systemic immune
activation occurs ↑ Endothelium (lining of blood vessels) activation
opens intercellular junctions (“leaky” blood vessels”)
↑ Inflammatory mediators
circulate throughout the body
Weight bearing joints (knee, hip &
lumbar/cervical facet joints)
sustain the highest mechanical
load & degenerate over time
Synovial fluid accumulates &
leads to joint edema (swelling)
↑ Blood flow carries heat
to affected joint tissues
Swelling
activates
joint
nociceptors
(damage
alarms)
Fluid
builds in
the
synovial
membrane
overnight
Edema
(swelling)
Warmth
Erythema
(redness)
Extra-articular
(body tissues
outside of
joints)
inflammatory
damage
± ↑
Inflammatory
markers (CRP,
ESR) & auto-
antibodies
(RF, ANA)
Movement (using the
joint) exacerbates the
mechanical forces
wearing down the joint
Pain with
movement
Pain relieved
with rest
Pain worse
with rest
Morning
joint stiffness
Movement
(using the
joint) pushes
fluid into
lymphatic
vessels
(cleaners)
Lymphatic
vessels
(cleaners)
need ↑ time
to reabsorb
↑ fluid
overnight
Pain relieved
with
movement
Joint stiffness
resolves ~1 hour
after waking
Authors:
Yan Yu
Mackenzie Trpcic
Reviewers:
Jennifer Au
Sean Spence
Martin Atkinson*
Catherine R Jarvis
* MD at time of
publication
Legend: Pathophysiology Mechanism
Sign/Symptom/Lab Finding Complications
Fragments of articular
(joint) cartilage trigger a
synovial (thin lining inside
of joints) inflammation
Inflammation causes
fluid to seep into the
synovial membrane
during inactivity
Joints stiffen
with rest
Movement (using
the joint) pushes
inflammatory fluid
back into lymphatic
vessels (cleaners)
Joint stiffness
resolves within
minutes of
movement
Published on www.thecalgaryguide.com
Inflammatory vs Degenerative Joint Disease: Pathogenesis & clinical findings
Inflammatory Joint Disease
The body’s immune system fails to discriminate between self and non-self
Auto-immune cells attack body tissues
↑ Synovial (thin lining inside of joints)
inflammation dilates blood vessels
↑ Endothelium (lining inside of
blood vessels) permeability
Synovial fluid accumulates &
leads to joint edema
(swelling)
Systemic immune
activation occurs
↑ Inflammatory mediators
circulate throughout the
body
Extra-articular
involvement
(body tissues
outside of
joints)
Elevated
inflammatory
markers (CRP,
ESR) & auto-
antibodies
(RF, ANA)
Degenerative Joint Disease
Abnormal
mechanics (e.g.,
poor posture,
weak stabilizing
muscles)
Repetitive/excess
stress on joints
Weight bearing joints (knee, hip &
lumbar/cervical facet joints)
sustain the highest mechanical
load & degenerate over time
Movement (using the joint)
exacerbates the mechanical
forces wearing down the
joint
Pain with
movement
Pain
relieved
with
rest
Authors:
Yan Yu
Mackenzie Trpcic
Reviewers:
Jennifer Au
Sean Spence
Martin Atkinson*
Catherine R Jarvis
* MD at time of
publication
Swelling activates
pain-sensitive joint
nociceptors
(damage alarms)
Pain worse with rest
Joint movement
pushes fluid into
lymphatic vessels
(body's clean-up
system)
Pain relieved
with movement
Legend: ↑ Blood flow carries heat to
affected joint tissues
Edema
(swelling)
Warmth
Erythema
(redness)
Fluid gradually builds in the
synovial membrane overnight
Morning joint stiffness
Lymphatic vessels
(body's clean-up system)
need ↑ time to reabsorb
↑ fluid that accumulated
overnight
Joint stiffness resolves ~1
hour after waking
Fragments of articular
(joint) cartilage trigger a
synovial (thin lining inside
of joints) inflammation
Inflammation causes fluid
to seep into the synovial
membrane during inactivity
Joints stiffen with rest
Moving the joint
physically pushes
inflammatory fluid back
into lymphatic vessels
(body's clean-up
system)
Joint stiffness resolves
within minutes of
movement
Pathophysiology Mechanism
Sign/Symptom/Lab Finding Complications
Published on www.thecalgaryguide.com
JOINT DISEASE: Inflammatory vs. Degenerative
Inflammatory Joint Disease
The body’s immune system fails to discriminate between self and non-self
Auto-immune cells attack body tissues
↑ Synovial (thin lining inside of the joint)
inflammation dilates blood vessels
↑ Endothelium (inner lining of blood
vessels) permeability
Synovial fluid accumulates &
leads to joint edema (swelling)
↑ Blood flow carries
heat to affected joint
tissues
Swelling activates
pain-sensitive joint
nociceptors
(damage alarms)
Fluid accumulates
progressively in the
synovial membrane
overnight
Edema
(swelling)
Warmth
Inflammatory pain
worse with rest
Morning joint
stiffness
Erythema
(redness)
Joint movement physically
pushes fluid back into
lymphatic vessels (body's
clean-up system)
Lymphatic vessels (body's
clean-up system) need ↑
time to reabsorb the ↑ fluid
that accumulated overnight
Inflammatory pain relieved
with activity
Joint stiffness resolves > 1hr
after waking
Legend: Mechanism
Sign/Symptom/Lab Finding Systemic
immune
activation occurs
↑
Inflammatory
mediators
circulate
throughout the
body
Extra-
articular
involvement
(e.g., skin,
eyes, lung,
heart,
kidneys) ±
abnormal
inflammatory
markers (CRP,
ESR) &
autoantibodi
es (RF, ANA)
Pathophysiology Complications
Degenerative Joint Disease
Abnormal mechanics or repetitive/excessive
loading stresses the joints
Joint structures degrade over time
Movement
(using the
joint)
exacerbates
the
mechanical
forces that are
wearing down
the joint
Pain with
movement
Pain relieved
with rest
Fragments of broken
articular cartilage
triggers a mild
synovial (thin lining
inside of the joint)
inflammation that
seeps fluid into the
synovial membrane
during inactivity
Joints stiffen with rest
Moving the joint
physically pushes
inflammatory fluid
back into lymphatic
vessels (body's clean-
up system) within
minutes
Joint stiffness resolves
within minutes of
movement
Published on www.thecalgaryguide.com
Authors:
Yan Yu
Mackenzie Trpcic
Reviewers:
Jennifer Au
Sean Spence
Martin Atkinson*
Catherine R Jarvis
* MD at time of
publication
The weight-
bearing joints
(i.e., knee, hip, &
lumbar/cervical
facet joints)
sustain the
highest
mechanical load
& degeneration
Distinguishing between Inflammatory and Degenerative joint disease
Inflammatory Joint
Disease
Auto-immune attack of body tissues, due to
failure of the body’s immune system to
discriminate between self and non-self.
Degenerative Joint
Disease
Repetitive, excess, or abnormal mechanical
forces on joints over time, leading to physical
breakdown of the joint.
Authors:
Yan Yu
Reviewers:
Jennifer Au
Sean Spence
Martin Atkinson*
* MD at time of
publication
Within joints, severe synovial inflammation
dilates local blood vessels, and causes the
vessel endothelium to be more leaky.
Accumulation of abundant
inflammatory synovial fluid
at rest or overnight
Swelling stimulates
joint nociceptors
Pain with rest
Moving the joint
physically pushes fluid
back into lymphatics,
relieving the painful
swelling.
Pain relieved with
motion
Legend: Overnight fluid
accumulation in the
synovial membrane
Morning stiffness
Lots of fluid, takes
more time (hours)
to be reabsorbed
by lymphatics
Stiffness resolves
after >1hr
Blood carries
heat and
looks red
Warm, Red,
Swollen
Joints
Pathophysiology Mechanism
Sign/Symptom/Lab Finding Inflammation is
oftentimes
systemic, not
localized
exclusively within
the joint (i.e. in
Rheumatoid
arthritis, Lupus,
etc)
Extra-articular
manifestations;
positive
inflammatory
markers (CRP,
ESR, RF, ANA)
Motion (using
the joint)
exacerbates the
mechanical
forces that are
wearing down
the joint
Fragments of
broken articular
cartilage triggers a
mild synovial
inflammation that
seeps fluid into the
synovial membrane
during inactivity
Pain with motion
(relieved by rest)
Joint stiffness
after inactivity
Moving the joint physically
pushes inflammatory fluid
back into lymphatics within
minutes.
Note: one big difference btw
the two is the degree of joint
inflammation (synovitis)
present in the joint capsule
Stiffness is short-lived,
quickly relieved by
movement
Published November1,2012 on www.thecalgaryguide.com
Larger, weight-
bearing joints tend to
bear the brunt of the
mechanical forces
Most commonly
affects the knee,
hip, and L/C-spine
facet joints
Complications" />
